Tackling health inequities and climate change

It’s common to hear that the impacts of climate change are unequally distributed — that those who contribute the least will suffer the most. It’s repeated frequently because, well, it’s true. There are three major factors behind this:
- Vulnerability
- Susceptibility
- Resilience
Vulnerability relies on varied levels of exposure between individuals or groups to things like:
- Air pollution
- Extreme weather, or
- Environmental toxins
Factors that influence vulnerability include zip code, living conditions, and behaviors. Susceptibility refers to a person’s predisposition to the harmful health effects of climate change and relies on factors like genetics or pre-existing health conditions that make an individual more likely to experience negative health effects from exposure. Resilience can rely either on people’s capacity to take protective precautions or their ability to recover from negative impacts. People, communities, and countries that have fewer resources (wealth, health infrastructure, education infrastructure, time, etc.) have a more limited capacity to adapt and recover. Combined, populations that have low resilience and high vulnerability are by and large low-income communities and communities of color.
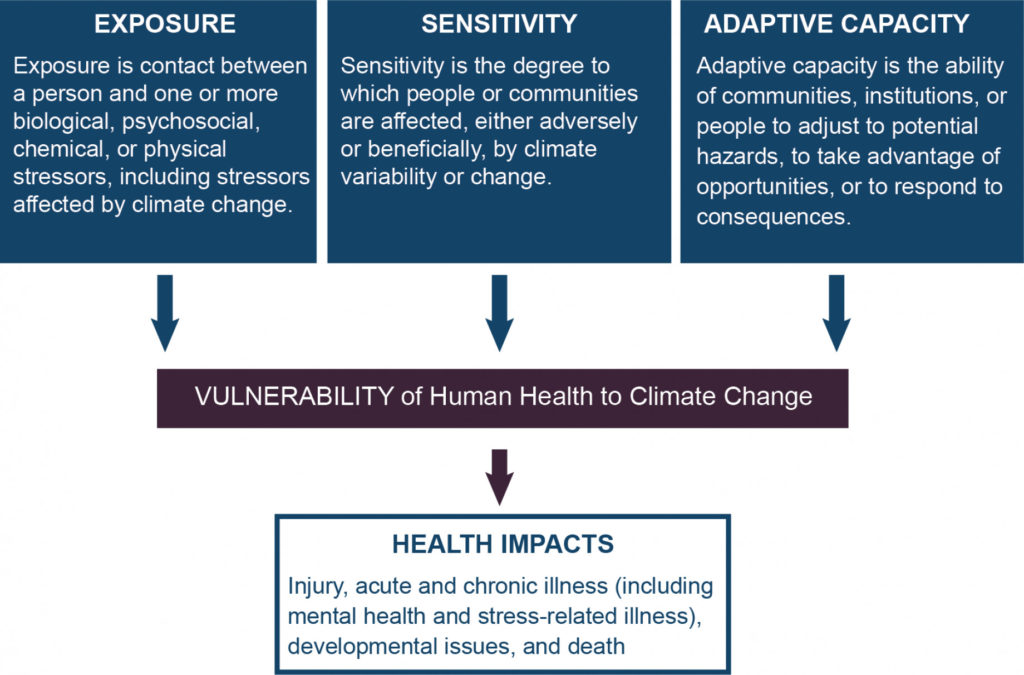
The figure below from the US Global Change Research Program Climate and Health Assessment help illustrate the interrelationships between climate, vulnerability, susceptibility, resilience, and social determinants of health effects.
Intersection of Social Determinants of Health and Vulnerability:
https://health2016.globalchange.gov/populations-concern
As per the US Global Change Research Program Climate and Health Assessment:
“Social determinants of health interact with the three elements of vulnerability. The boxes on the left provide examples of how social determinants of health are associated with each of the elements of vulnerability. Increased exposure, increased sensitivity, and reduced adaptive capacity all affect vulnerability at different points in the causal chain from climate drivers to health outcomes (middleboxes). Adaptive capacity can influence exposure and sensitivity as well as influence the resilience of individuals or populations experiencing health impacts by affecting access to care and preventive services. The boxes on the right give examples of the implications of social determinants on increased exposure, increased sensitivity, and reduced adaptive capacity.”
What health inequities look like through the lens of climate change
Disproportionate impacts of health inequities are not happenstance but stem from disparities in:
- The distribution of money and power
- Discriminatory practices and policies
- Historical disinvestment
- Structural racism
- Environmental injustice, and
- Unequal access to health care
Environmental justice communities are affected by environmental and socioeconomic factors that work together to produce persistent health disparities. These communities are more likely to have low tree cover and a lack of green space, which contributes to higher temperatures. The rate of heat-related deaths for Black Americans is 150-200 percent greater than that of white Americans.
Additionally, the disproportionate distribution of power plants and refineries in low-income communities and communities of color increases the likelihood of these communities being affected by air pollutants. Polluted air has been linked to lung disease, asthma, cardiovascular disease, and other health conditions.
Pre-existing conditions and lower levels of resilience put members of environmental injustice communities at higher risk for adverse health impacts during climate events, including hurricanes and heatwaves. Pre-existing conditions can include diabetes, cardiovascular disease, and other immune-compromising illnesses.
Including marginalized community leaders in policy discussions to mitigate climate change fueled health inequities
The close tie between health and climate drivers means that climate mitigation, adaptation, and resilience measures have significant health benefits. Environmental health policies and interventions should therefore be driven through an equity lens. If these policies are implemented equitably with input from marginalized communities, climate policy can close health gaps and address historical inequities.
Devin O’Donnell is an MPH candidate at the Boston University School of Public Health, focusing on community health and human rights. She is interested in the intersection of climate change and health, more specifically, how community mobilization and cohesion are necessary for mitigation and adaptation efforts. Devin is working with the BUSPH Program on Climate and Health and the American Red Cross in these realms. In her free time, you can find Devin reliving her bakery days or exploring the nearby trails.
Quinn Adams is a PhD student in the Department of Environmental Health at the Boston University School of Public Health. She also received her MS in Climate and Health at BUSPH. Quinn is interested in understanding the influence of climate change and extreme weather events on human health outcomes, and has a particular interest in the impact of climate on emerging infectious diseases and disease transmission. Previously, Quinn held positions working on environmental health issues at the National Caucus of Environmental Legislators (NCEL) and the Association of Public Health Laboratories (APHL) in Washington, DC.





